
Radar | Dec 10,2022
Jan 7 , 2024
By Peter Singer
When vaccines for COVID-19 became available, governments’ highest priority was to get them approved as quickly as possible, to save millions of lives. Regulatory authorisation of a new, low-cost malaria vaccine, recommended by the World Health Organization (WHO) in October, deserves to be treated with the same degree of urgency.
In 2021, malaria caused 619,000 deaths, 77pc of which were children under five, and 96pc of them in Africa.
But now, after decades of research – and several false dawns – a malaria vaccine known as "R21/Matrix-M" (henceforth just R21) is effective in 70pc to 78pc cases. Although three doses are required before that level of protection is reached, and a booster is needed one year later, the vaccine, developed at the University of Oxford and the Serum Institute of India, is cheap. It can be produced for two dollars to four dollars for a dose – comparable to the cost of other childhood vaccines.
Adding costs for delivery and administration, we can say that R21 costs approximately five dollars per dose. A recent study indicates that fully vaccinating eligible children in areas where malaria is prevalent would save more than 600 lives per 100,000 children vaccinated, as well as prevent nearly 200,000 clinical cases of malaria (because once someone gets malaria, it is likely to recur). This suggests that the deaths of hundreds of thousands of children could be prevented for roughly 3,300 dollars per life saved.
In October, R21 was recommended by the World Health Organisation (WHO). It now needs to go through the WHO’s prequalification process and receive the WHO’s Strategic Advisory Group of Experts on Immunisation recommendation. Then, a broad international rollout can begin.
Children eligible for R21 are between five months and three years old. About 80 million eligible children live in malaria-prone regions of Sub-Saharan Africa. To give them all three doses of the vaccine in 2024 would require 240 million doses, followed by a further 80 million boosters in 2025. After that, with the backlog of currently unvaccinated children dealt with, the roughly 30 million children born every year would need 120 million doses. This would save about 450,000 lives per year.
Saving a life for a bargain.
In the United States, Medicare covers the cost of kidney dialysis for patients over 65 who would otherwise die while awaiting a transplant. Fifteen years ago, economists from Stanford and Wharton calculated that the average cost per quality-adjusted year of life gained by this coverage was 129,000 dollars. Adjusting that figure for inflation (and overlooking that medical costs have risen faster than other prices) takes it to 182,000 dollars – and that is for one extra year of life.
By comparison, if we conservatively estimate that the children saved by vaccination against malaria have a life expectancy of 50 years, the cost per year is 66 dollars.
Even when judged by global, rather than American, standards, saving a life for 3,300 dollars is an exceptionally good value. The most cost-effective evidence-backed programs that leading charity evaluator GiveWell has been able to find cost roughly 3,500 dollars to 5,500 dollars for a life saved. For example, the Against Malaria Foundation, one of The Life You Can Save’s top charities, distributes bed nets to protect children against malaria. Although each net costs only a few dollars, distributing enough to save a life costs over 4,000 dollars.
When vaccines for COVID-19 first became available, governments’ highest priority was to get them through the regulatory process. The US Food & Drug Administration typically takes about 10 months to authorise the use of a new vaccine, but it approved the use of the Pfizer vaccine in a breathtaking 21 days, and authorisation for Moderna’s vaccine took just 19 days. WHO prequalification usually takes 270 days after the WHO recommends a vaccine. That is an unacceptable delay. The WHO should accelerate its process and tell the public how quickly it can complete prequalification.
1Day Sooner was founded to represent people who wanted to volunteer to participate in human challenge trials to accelerate vaccine development. When the organisation was established in March 2020, its focus was a vaccine against COVID-19: getting it out one day sooner would, quite literally, save thousands of lives. Many of the organisation’s staff and a high proportion of the volunteers were effective altruists.
The organisation’s original mission has broadened to promote the efficient development of life-saving medical research and the speediest and most equitable distribution of its products. As part of that broader mission, 1Day Sooner set up 1Day Africa to promote vaccination on the continent by strengthening Africa’s scientific capacity and ability to manufacture vaccines locally. Now, 1Day Africa is concerned that the WHO and national governments are not assessing the safety and effectiveness of the new malaria vaccine with the same urgency as they assessed the COVID-19 vaccines.
As a result, the organisation is pressing for the production of as many doses of R21 as possible in 2024 and getting those doses into the arms of children as quickly as possible to prevent millions of malaria cases and save hundreds of thousands of lives. Some of the relevant facts are in dispute, including how long the WHO’s prequalification process needs to take, and how quickly the necessary quantity of doses can be produced.
But one thing should be clear: failing to save the lives of African children when that can be achieved for as little as 3,300 dollars each would render hollow our lofty rhetoric about the equal worth of every human life.
PUBLISHED ON
Jan 07,2024 [ VOL
24 , NO
1236]


Radar | Dec 10,2022

Sunday with Eden | Jul 10,2021

Sunday with Eden | Apr 11,2020

Life Matters | Feb 04,2023

Life Matters | Nov 29,2020

Sunday with Eden | Dec 21,2019

Editorial | Aug 22,2020

My Opinion | Apr 09,2023

Fortune News | Jun 22,2019

Agenda | Sep 19,2020

My Opinion | 108833 Views | Aug 14,2021

My Opinion | 105226 Views | Aug 21,2021

My Opinion | 104038 Views | Sep 10,2021

My Opinion | 103324 Views | Aug 07,2021

Jul 13 , 2024 . By AKSAH ITALO
Investors who rely on tractors, trucks, and field vehicles for commuting, transportin...

Jul 13 , 2024 . By MUNIR SHEMSU
The cracks in Ethiopia's higher education system were laid bare during a synthesis re...

Jul 13 , 2024 . By AKSAH ITALO
Construction authorities have unveiled a price adjustment implementation manual for s...

Jul 13 , 2024
The banking industry is experiencing a transformative period under the oversight of N...

Jul 20 , 2024
In a volatile economic environment, sudden policy reversals leave businesses reeling...

Jul 13 , 2024
Policymakers are walking a tightrope, struggling to generate growth and create millio...

Jul 7 , 2024
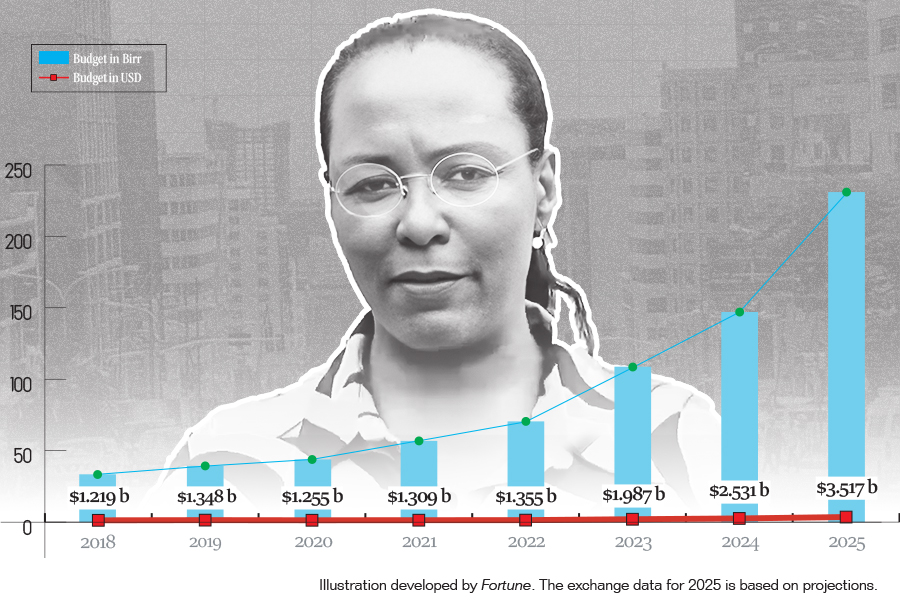
The federal budget has crossed a symbolic threshold, approaching the one trillion Bir...

Jun 29 , 2024
In a spirited bid for autonomy, the National Bank of Ethiopia (NBE), under its younge...
Jul 21 , 2024 . By TIZITA SHEWAFERAW
Mayor Adanech Abebie's Administration faced an audit report that unveiled a startling...

Jul 21 , 2024 . By AKSAH ITALO
Brook Taye (PhD), director general of the Ethiopian Capital Market Authority, has tak...

Jul 21 , 2024 . By AKSAH ITALO
Ethiopia's horticulture, a major source of foreign currency and employment, is facing...

Jul 21 , 2024 . By AKSAH ITALO
Commercial banks are now permitted to acquire equity shares in capital market service...